What to Know About Changing Medicare Costs in 2021
Healthcare in the US is a very tenuous subject. Millions of Americans struggle every year with healthcare costs. 2020 has been a very stressful year for most, and worrying about healthcare coverage shouldn’t be an extra stress. For older Americans, health insurance is a must, so Medicare is there to help. Medicare is the federal health insurance program created in 1965 to provide health coverage for Americans aged 65 and older. Approximately 12 percent of the Medicare population is aged 85 or older.
More than 61 million Americans are currently covered by Medicare, and funding for the program accounted for 14 percent of federal spending in 2018.
Generally speaking, you are eligible for Medicare if one of the following applies:
- you are 65 years old, and have been a legal permanent US resident for at least five continuous years.
- you are under 65 and have amyotrophic lateral sclerosis (ALS) – also known as Lou Gehrig’s Disease – or end-stage renal disease (ERSD); or
- you aren’t yet 65, but have been entitled to Social Security Disability benefits for at least 24 months.
In order to get Medicare Part A with no premium, you also need to have paid into the Medicare system. This means that you or your spouse (or a parent, if you’re enrolling as a disabled child) must have worked for at least ten years prior to enrolling in Medicare. If not, you’re still eligible, but will have to pay a premium for Medicare Part A.
Here are the changes coming to Medicare in 2021.
The Part B deductible is $203 in 2021

Rising deductible. Shutterstock.
In 2020, the Part B deductible was only $198, which isn’t a huge change. Some people won’t need to worry about this incremental increase too much though. Some enrollees have supplemental coverage that pays their Part B deductible. This includes Medicaid, employer-sponsored plans, and Medigap plans C and F. But Medigap plans C and F can no longer be sold to newly-eligible enrollees as of 2020. But if you already have a Medigap plan, don’t worry – you’re basically grandfathered in, you get to keep them. People who were already eligible for Medicare prior to 2020 can continue to purchase them.
Many Medicare Advantage plans have low copays and deductibles that don’t necessarily increase with the 2021 Part B deductible, so their benefits designs have had different fluctuations over the last few years.
The High-Income Brackets will be Higher in 2021

Increased income tax bracket. Shutterstock.
The high-income brackets were introduced in 2007 for Part B and in 2011 for Part D, and for several years they started at $85,000 ($170,000 for a married couple). But the income brackets began to be adjusted for inflation as of 2020, with the start of the “high-income” range increasing to $87,000 per year ($174,000 for a married couple). For 2021, these thresholds have increased to $88,000 for a single person and $176,000 for a married couple. If you’re wondering how this works, it is based on income tax returns from 2019. They usually go off your most recent tax returns and since you won’t have filed your 2020 taxes yet, your 2019 is the best reference. If your income has changed since 2019, you can also file an appeal.
For 2021, the Part B premium for high-income beneficiaries ranges from $207.90/month to $540.90/month, depending on income. This is changing from 2020 to a range of $202.40/month to $491.60/month.
People with ESRD can join Medicare Advantage plans
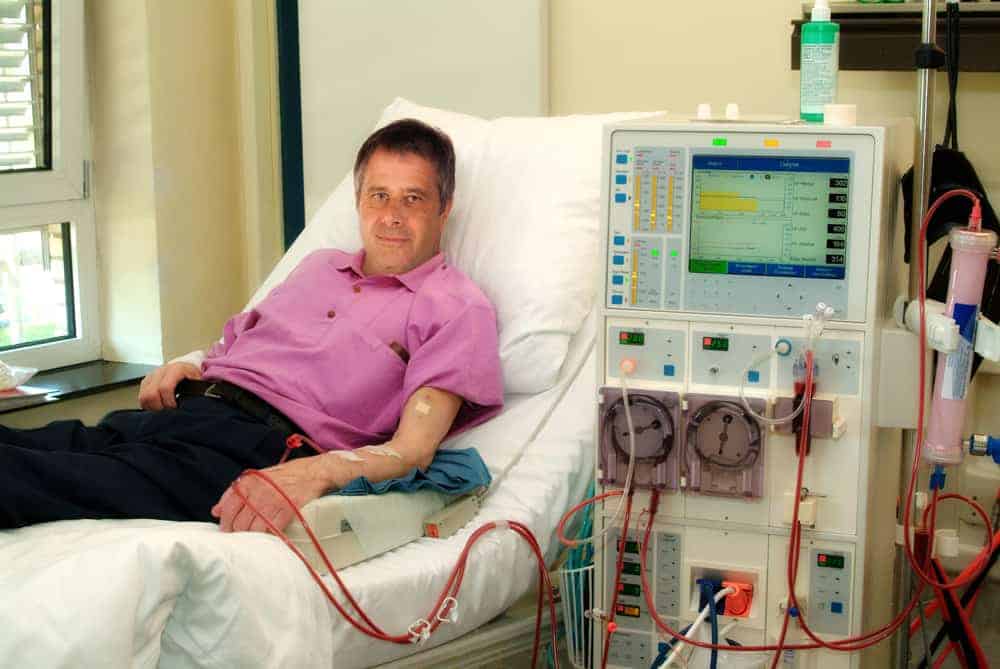
Man getting dialysis with End Stage Renal Disease (ESRD). Shutterstock.
For years, those suffering with End Stage Renal Disease (ESRD) would not be eligible for Medicare coverage plans. In 2021, that’s all about to change.This is thanks to the 21st Century Cures Act, which gives people with ESRD access to any Medicare Advantage plan in their area as of 2021. This will create more affordable healthcare opportunities to those suffering with ESRD. A patient with end-stage renal failure must receive dialysis or kidney transplantation in order to survive for more than a few weeks. Patients may experience a wide variety of symptoms as kidney failure progresses. As expected, these costs for treating ESRD add up fast. Of course there are still some limitations. Many people suffering with this can opt for the Medigap coverage. Medicare Advantage plans do have a cap on out-of-pocket costs, as described below. So for ESRD beneficiaries who cannot obtain an affordable Medigap plan, a Medicare Advantage plan could be a viable solution, as long as the person’s doctors and hospitals are in-network with the plan.
The maximum out-of-pocket limit for Medicare Advantage plans is increasing

Maximum out of pocket is increasing in 2021. Shutterstock.
Medicare Advantage plans are required to cap enrollees’ out-of-pocket costs for Part A and Part B services. However, Original Medicare does not have a cap on out of pocket costs. Keep in mind, this cap does not include the cost of prescription drugs. Prescription drug coverage is available under Medicare Part D – even when it’s integrated with a Medicare Advantage plan.
For the last several years, the cap has been $6,700, although most plans have had out-of-pocket caps below that level. For 2021, the maximum out-of-pocket limit for Medicare Advantage plans is increasing to $7,550. Once again, this is plus out-of-pocket costs for prescription drugs. Most plans will likely continue to have out-of-pocket caps below the government’s maximum, but the allowable increase for 2021 is fairly significant.






